Breakthrough Prostate Cancer Treatment Uses Ultrasound Waves To Eliminate Tumors By Elias Marat for Natural Blaze
Doctors have made a tremendous step forward in the fight against prostate cancer, using targeted ultrasound pulses to successfully eliminate the disease entirely in 65 percent of cases with few side effects.
The new method, detailed in a study presented at the annual meeting of the Radiological Society of North America (RSNA), could be a promising alternative to surgery.
Prostate cancer is the most common cancer among men, second only to skin cancer. It is also the second leading cause of cancer deaths among men in the United States. According to the American Cancer Society (ACS), an estimated 174,650 men in the U.S. will be diagnosed with prostate cancer in 2019 alone.
Traditional treatments involving surgery and radiation have proven challenging due to their life-altering effects, namely leaving subjects impotent, incontinent, or with bowel dysfunctions. An estimated 3 million survivors of prostate cancer are alive in the U.S. today.
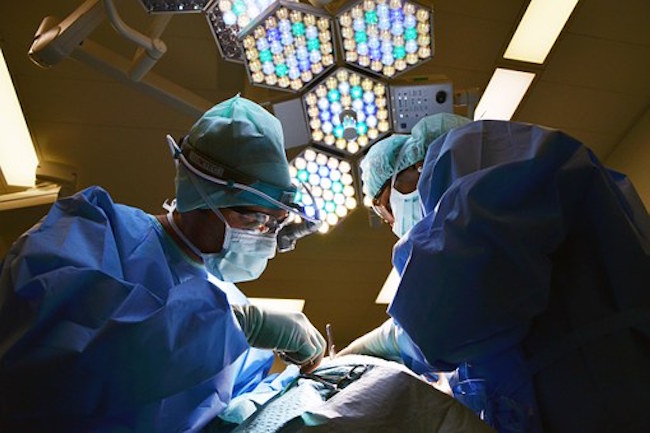
Yet the revolutionary new technique avoids such risks by relying on a rod-shaped device that is inserted into the urethra and uses magnetic resonance or MRI to focus precise ultrasound pulses on tumors, heating and destroying them while leaving the surrounding areas entirely unharmed.
The minimally invasive method, called MRI-guided transurethral ultrasound ablation—or TULSA—was used on 115 men suffering localized prostate cancer.
According to researchers, in 80 percent of the cases most signs of cancer were eliminated, while all signs were gone in 65 percent of the cases after one year. No bowel complications were reported, overall, while most men saw their blood-antigen markers for prostate cancer reduced.
Results of the TULSA trial show clinically significant prostate cancer was eliminated in 80% of study participants, and 65% had no evidence of cancer at biopsy after one year. #RSNA19 #SIR #UCLA Radiology https://t.co/vui6wZRPOG via @medical_xpress
— Steven S. Raman MD, FSAR, FSIR (@StevenSRaman_MD) December 2, 2019